A routine mole check helps to identify and to treat skin cancer early. The dermatoscope (or dermoscope) is thereby a very helpful tool to avoid unnecessary operations and to identify skin cancer early in the same time.
A (digital) dermatoscope is an effective tool to recognize melanomas and other types of skin tumors at an early stage. As for any other types of cancer, early diagnosis is crucial for survival. Features that are only visible using this tool helps the doctor to discriminate between benign (i.e. harmless) from cancerous lesions more precisely. Therefore, unnecessary operations can be avoided when the tool is used properly.
Besides the inspection and follow up of suspicious moles using a digital dermatoscope (or dermoscope), Prof. Dr. Okamoto offers a Bodyscan, where the entire body can be fotographed and saved for future comparisons.
Moles are benign lesions of the skin. They might appear and change in number and size throughout the entire life. Sun and artificial UV light such as sun beds are the best known triggers of moles. Several studies have shown that the number of moles correlates with melanoma: the more moles the higher the risk of melanoma. Therefore, a regular mole check is recommended for individuals with many moles.
However, in case of a suspicious lesion, only a surgical removal can provide a reliable diagnosis. At Prof. Dr. Okamoto’s office, diagnosis and surgery of skin tumors surgery of skin tumors are offered routinely.
For arranging an appointment, please contact our office by phone, per E-Mail to ordination@hautarztokamoto.at or use the online-form.
Mole check in Vienna by Prof. Dr. Okamoto
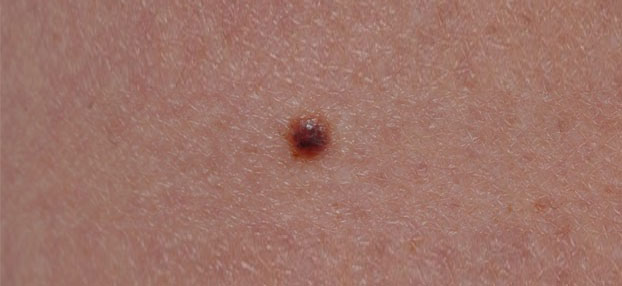
A mole check helps to identify skin cancer at an early stage and to prevent progression of a potentially unfavorable disease. Many moles are easy to recognize, but some might have a more irregular shape or color. In such situations, dermatoscopy helps to specify the diagnosis before surgery.
Dermatoscopy
A dermatoscope or also known as “dermoscope” is a tool that enables the viewer to see features that are invisible to the naked eye. These features are indicative of whether the analyzed lesion is harmless or cancerous. Typically, such an instrument consists of a magnifier (typically x10), a light source (polarized or non-polarized) and a transparent plate. The advantage of using a dermatosope is that it enables a more precise assessment than just by looking with a magnifying lens. This is because by applying the transparent plate on the skin, deeper layers become visible comparable to a goggle to snorkelers or divers. Therefore, using this technique the certitude of the diagnosis is increased without removing the lesion. However, should uncertainty remain, the lesion should be either removed or observed with digital dermatoscopy.
Digital dermatoscopy
In case of a “borderline” lesion, follow-up using digital dermatoscopy can be a reasonable alternative to surgery. Images taken by dermatoscopy are saved in a computer, and changes of the lesion can be monitored in follow up examinations. This method also known as sequential dermatoscopy allows to assess potential changes with time, which provides additional crucial information about the lesion. While most moles are recognized undoubtedly, this method enables a more precise assessment as the lesions are observed several times at different time points. Therefore, early changes occurring at an early stage can be monitored objectively.
Bodyscan
Besides the inspection and follow up of suspicious moles using a digital dermatoscope (or dermoscope), Prof. Dr. Okamoto offers a Bodyscan, where the entire body can be fotographed and saved for future comparisons. This method provides the advantage of detecting changes even of unconspicuous lesions. Moreover, new lesions that emerge over time can be detected more reliably. This is of importance as skin cancer does not necessarily develop on pre-existing lesions. Whole body scan is particularly useful for patients at higher risk such as those who have been already diagnosed for skin cancer in the past, with high number of moles or a positive family history of melanoma.
Dermatologist Prof. Dr. Okamoto provides information on mole checks in Vienna (Austria). Please call for appointments by phone, or send us an e-mail to ordination@hautarztokamoto.at. Alternatively, you are welcome to fill out a contact form.
The “ABCDE rule”
Melanoma is the most dangerous skin cancer type with a continuous increase in incidence world wide. This “rule” was established to help lay people to identify suspicious lesions to prevent deaths caused by melanoma. It serves rather as a mnemonic than established criteria to identify melanomas and is composed of the following features.
A = Asymmetry
Common and benign moles are either round or ovally shaped and can therefore be split in 2 identical halves. They are usually symmetric. Melanomas show irregular growth leading to rather asymmetric forms.
B = Border
Moles show a clear demarcation to the surrounding skin. The border between the mole and the surrounding skin is clear. Borders of melanomas are not always that clear. They can be diffuse or frayed.
C = Color
The more color a lesion has, the more likely becomes the diagnosis of melanoma (“american flag sign”=if a lesion has red, white and blue parts beside brown)
D = Diameter
Obviously, cancerous lesions grow faster and without limitation compared to benign lesions which are characterized by limited growth. Therefore, the larger a lesion in general, the more likely becomes the diagnosis of melanoma. The cut-off size of a “large” lesion is arbitrary but currently the diameter of 6mm is commonly accepted.
E = Elevation
In case of an elevation of a lesion or parts of it makes the diagnosis of melanoma more likely.
Should you find one or more of the above mentioned criteria, a consultation at a dermatologist is recommended.
How often should I have my moles checked?
A general recommendation applicable for everyone is very difficult as each person is individual. Therefore, the risk for every person should be assessed individually. Following characteristics are established risk factors of melanoma:
- previous diagnosis of melanoma
- melanoma of a related family member
- many moles
- signs of sun damage (particularly on the back)
- light skin complexion with a low tendency to tan
If one of the above mentioned characteristics apply to you, a regular mole check should be done at least once per year. In a case of a recent diagnosis of melanoma, the frequency should be increased to up to 4 times per year (i.e. every 3 months). The frequency depends on further details of the primary tumor as well as other signs of skin damage or tumors (i.e. non-melanoma skin cancer). Remember, a routine check is also recommended for people with signs of actinic damage such as age spots or solar lentils.
Contact Prof. Dr. Okamoto
For appointments, please contact us by phone, or via E-Mail at ordination@hautarztokamoto.at or contact form.
