Atopic Dermatitis (also known as neurodermitis) is a chronic inflammatory disease of the skin as part of a general overreaction of the body, mostly to external factors (atopy). Atopy describes a systemic reaction affecting numerous organs such as the eyes (conjunctivitis), nose (rhinitis) and lungs (asthma). It can begin very early in life. Sometimes, patients suffer from atopic dermatitis or neurodermitis since their birth. This skin disease is characterized by dry, scaly plaques. The single lesions are also called eczema.
For arranging an appointment for treatment of atopic dermatitis or neurodermitis in Vienna, please contact our office by phone, email (ordination@hautarztokamoto.at) or use the online-form.
Information about atopic dermatitis by dermatologist Prof. Dr. Okamoto in Vienna (Austria)
Characteristic symptoms of atopic dermatitis
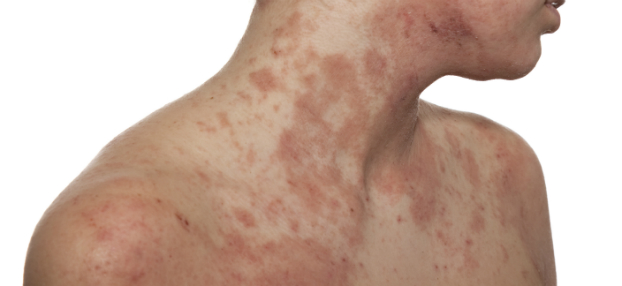
Atopic dermatitis is characterized by reddening of the skin with scales and sometimes even blisters (particularly on the hands and feet). Although the intensity can vary, there are specific areas that are commonly affected and characteristic for the disease. They include the head, cheeks, chin, elbows, hollow of the knees, neck and the wrists for neonates. Later, besides elbows and the knees, arms, legs and hands (fingers) are commonly affected. External factors such as the cold, fluids (such as saliva, sweat, detergents, etc.), dry air and allergens are common triggers of this skin disease.
Pruritus (itch) is the dominating and most irritating symptom of atopic dermatitis, which limits both quality of life as well as performance at school or work. Instantly, one can hardly resist to scratch but scratching even deteriorates the symptoms. Often, scratching causes damage on the surface of the skin leading to erosions, bleeding and infections. The inflammation can then spread and affect multiple areas of the skin leading to the typical affection of atopic dermatitis.
Allergic sufferers often complain about eczema after or during an allergic episode or season. Desensitization against allergens can help to suppress atopic dermatitis. Besides food allergies, some nutrients can sometimes enhance the itch as they might irritate the skin or intensify pruritus (e.g. citrus fruits). The course is generally chronic, and the condition can last for several months to years with changing intensities.
Causes and triggers
Atopic dermatitis is for the most part inherent. Often, parents or siblings suffer from the same disease. Several external factors can trigger an inflammatory (over-)reaction of the immune system, which can lead to allergic rhinoconjunctivitis (hey fever), allergic asthma or even to an urticarial rash. Emotional conditions (“stress)” are also known to provoke or enhance atopic dermatitis (therefore the original name “neurodermitis”).
Therapy
In most cases, diagnosis is unambiguous and can be made by a dermatologist without any extensive effort. In case of doubt, a biopsy of the affected skin can be helpful. In an acute phase, a topical treatment with cortisone ointments is the treatment of choice. To avoid relapses after treatment, lubrication of the skin is crucial. A frequent replenishing with medication-free ointments avoids the use of cortisone. Additionally, the trigger should be recognized by a detailed anamnesis: when did the first episode occur, when and where did the symptoms repeatedly appear, are there any known allergies, etc. Further analyses and allergy tests can reveal the trigger, which is helpful for prevention as well as for finding the specific treatment (desensitization).
As described above, allergen specific desensitization after appropriate testing reduces the frequency of relapses. Additionally, materials that dry out or irritate skin should be avoided. Also, as psychological or emotional stress tends to affect skin, sufferers from atopic dermatitis should be aware of the effect of mental health on their skin condition.
Dermatologist Prof. Dr. Okamoto informs about prevention of eczema and atopic dermatitis
In brief, Univ. Prof. Dr. Okamoto gives you tips as a dermatologist to prevent Ekzems and atopic dermatitis (neurodermitis):
- shower than bath
- lubrication (oily) than moisturizer
- wear cotton than wool
- overheated rooms in winter are “poison” for the skin
- do not scratch, instead use ointments
For further information about skin care in winter visit: Tipps for skin care in winter
Contact Prof. Dr. Okamoto
For appointments, please contact us by phone, or via E-Mail at ordination@hautarztokamoto.at or contact form.
