Erysipelas is a serious skin disease. A delayed or insufficient treatment leads to necrosis (death of the tissue) and eventually to the spread of the infection into the blood circulation, leading to sepsis. Once the bacteria has spread, a septic shock syndrome might be the consequence requiring treatment in an intensive care unit. Spontaneous remissions have been observed in cases with minor severity but relapses are common if not treated which require even extended therapy with antibiotics.
For arranging an appointment for treatment of eczema in Vienna, please contact our office by phone, email ordination@hautarztokamoto.at or use the online-form.
Erysipelas is a serious disease of the skin, characterized by an intensive reddening (“rubor” in latin), heat (“calor” in latin), pain (“dolor” in latin) and swelling (“tumor” in latin). This acute inflammatory disease is caused by a bacterial infection (mostly streptococci) of the skin. Commonly affected areas are the arms, legs and the face.
Information about Erysipelas by Prof. Dr. Okamoto (dermatologist in Vienna)
Symptoms

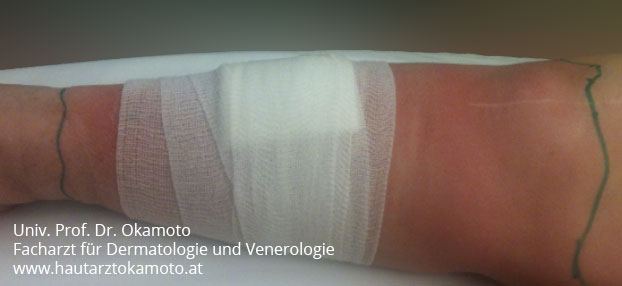
Characteristic features of this skin disease is a rather rapid enlargement of the erythematous (red) skin lesion which can reach a considerable size within a few days (see foto). The border or edge is sharply demarcated, and adjacent lymph nodes are often swollen and sensitive as a sign of immune response and the spread of the inflammation following lymph vessels. Sometimes, a red line can be seen from the border of the lesion indicating an inflammation of a lymph vessel, also known as lymphangitis. In the center of the red lesion which feels swollen, warm, hardened and painful, a (small) injury or even an ulcer can be found as the source of the infection. Typically, the entire body responses to this bacterial infection with high fever, shaking, chills, fatigue, headache and general weakness.
Low immunity, impaired vascular situation or otherwise weakened physical conditions can lead to more severe conditions. These include an affection of a large area (such as an entire limb), blistering and general deterioration requiring stabilization of circulation and monitoring of organ functions.
It is of upmost importance to start early with antibiotic treatment to avoid the spread to the surrounding tissue and organs. Once the tissue has died (necrotizing fasciitis), the only cure is urgent surgery.
Cause of Erysipelas
The most common cause of erysipelas is an infection of the skin with ?-hemolytic group A streptococci (Streptococcus pyogenes). The bacteria invade the skin through an injury which can be small and hardly visible such as a scratch. Certain skin conditions can facilitate the invasion such as epidermomycosis (fungal infection, tinea, “athlete feet”) or insect bites.
Once they have invaded the skin, the germs start to proliferate and to spread in the neighboring tissue. The immune system responses to this invasion, causing a massive inflammation of the skin as well as the neighboring lymph nodes.
Who is at risk?
Although everyone can acquire an erysipelas, children and older individuals are more likely to develop erysipelas. Risk is increased in patients with edemas (such as lymph edemas after mastectomy or edemas of the legs due to venous insufficiencies), diabetes, alcoholism, injuries and severe immune deficiencies or systemic diseases such as AIDS or cancer.
Diagnosis
 A specialist recognizes an erysipelas “clinically”, i.e. by its typical appearance and the systemic symptoms of the patient. A blood draw confirms the inflammatory disease by elevated C-reactive protein (CRP) levels and leucocyte counts.
A specialist recognizes an erysipelas “clinically”, i.e. by its typical appearance and the systemic symptoms of the patient. A blood draw confirms the inflammatory disease by elevated C-reactive protein (CRP) levels and leucocyte counts.
Following diseases should be distinguished from erysipelas:
- (allergic) contact dermatitis
- stasis dermatitis
- phlebitis
- insect bites (bees, wasps)
- Bursitis and arthritis/li>
- erysipeloid
Therapy
Intensive antibiotic treatment is required for the duration of approximately 14 days. The definite duration depends on the response of the patient to the treatment. I.v. infusions should be preferred to oral administration as they are more effective. Bed rest is required and an elevated position of the affected area such as leg or arm eases the pain and helps to reduce inflammation and swelling. Additionally, symptomatic treatment help to reduce fever and pain. In early stages and in otherwise healthy patients, the treatment can be performed at home. For medium to severe conditions, inpatient treatment is inevitable. In case of an insufficient duration or dosage of the treatment, erysipelas tend to reoccur requiring an extended treatment.
Dermatologist Prof. Dr. Okamoto informs about erysipelas
Prof. Dr. Okamoto, expert on skin diseases in Vienna, provides tipps about erysipelas also on netdoktor.at.
Erysipelas is a serious disease which can lead to life threatening conditions if not treated appropriately, particularly in individuals with co-morbidities such as heart failure. The aim of the treatment is sustainable remission.
Contact Prof. Dr. Okamoto
For appointments, please contact us by phone, or via E-Mail at ordination@hautarztokamoto.at or contact form.
