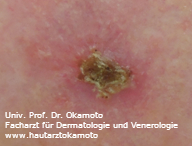
Figure 1: example of an ulcerating squamous cell carcinoma
Squameous cell carcinoma of the skin or briefly SCC is grouped together with basal cell carcinoma (BCC) as “non-melanoma skin cancer”. This grouping is disputed controversially, but it reflects some common features of SCCs and BCCs: they are commonly light colored and metastasis is rare after complete excision of the tumor.
Origin of Squameous cell carcinoma
SCCs originate from keratinocytes which forms more than 90% of the epidermis. Ultraviolet radiation of the sun is known to cause DNA breaks in the cell nuclei leading to transformation of the affected cells. The relation of sun exposure and SCC risk is linear, making cumulative sun exposure the most important external risk factor of SCCs. The more often someone is exposed to the sun, the higher the risk of developing SCCs.
For arranging an appointment for treatment of a Squameous cell carcinoma (SCC) of the skin in Vienna, please contact our office by phone +43 1 40114/5701, email ordination@hautarztokamoto.at or use the online-form.
Feartures – how do Squameous cell carcinomas look like?
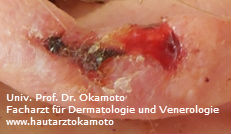
Figures 2: example of an ulcerating squamous cell carcinoma
In contrast to melanomas, SCCs are usually skin colored. They can evolve from precancerous lesions such as actinic keratosis or superficial forms such as Morbus Bowen. Actinic keratosis are sometimes hardly visible but are characterized by a rough, somewhat raspy surface (like a sandpaper). They are rather smaller in size but can occure multiple in the vicinity of usually unprotected areas such as forehad and the dorsum of the hand. A so called Morbus Bowen is better demarcated and rather bigger in size. It is flat and does not cause any symptoms. In case of an invasive SCC, the tumor starts to become elevated (thicker), eventually forming an ulcer (see figures 1 and 2).
Prevention
For SCCs, a consistent or continuous protection against the sun should be regarded. SCCs and their precursor lesions develop mostly – almost exclusively – on areas that are not covered by clothing and therefore are continuously exposed to the sun. Also, affected patients are usually elderly. Someone with a sun sensitive skin sensitive (easily burn and hardly tan) and a record with long hours staying under the sun frequently are at increased risk. Sun protection should not only include the regular use of sunscreen with sufficient sun protecting factors (ideally SPF 50, also in winter!) but also clothing that provides additional protection such as a hat or long sleeves and avoiding direct sun exposure for a long time.
Treatment (as of March 2016)
In case of SCCs not all lesions need to be surgically treated. Depending on the size and the stage of the tumor, alternative treatment options are available. For superficial lesions such as actinic keratosis and Morbus Bowen, freezing with liquid nitrogen has been used regularly. The doctor applies liquid nitrogen on the lesion and provokes a blister. With the blistering, the lesion is lifted from the skin and falls off by itself. Recently, self applied crèmes are available for larger or multiple superficial lesions. Please note that only superficial lesions should be treated with non surgical methods. Whether a lesion is superficial or invasive can only be determined by a small biopsy. After treatment, a follow up in regular interval is recommended. If surgery is required, one should make sure that the entire lesion was removed (i.e. the tumor is surrounded by healthy tissue or in latin “ in toto”). Seeding of SCCs into distant organs (metastasis) is very rare and occur only in very advanced stages.
Common non-cancerous tumors of the skin
Fortunately, most alterations on the skin are benign and do not require treatment. Those are the most common types of benign lesions:
- moles
- seborrhoic keratosis (“age spots”)
- hemangiomas
- lipoma
- warts
Please note
The content of this homepage is intended to help patients to obtain basic information about the above described topics and does not claim to be complete. Diagnosis and therapy is individual and can differ in certain circumstances from the above described. In case of any doubts or further questions, please ask your doctor.
For more information, please visit sonneohnereue.at or www.cancer.org/acs/groups/cid/documents/webcontent/003063-pdf.pdf
Contact Prof. Dr. Okamoto
For appointments, please contact us by phone +43 1 40114/5701, 5702 or 5703, or via E-Mail at ordination@hautarztokamoto.at or contact form.
